NUHS Institutions will NEVER ask you to transfer money or disclose bank details over a call.
If in doubt, call the 24/7 ScamShield helpline at 1799, or visit the ScamShield website at www.scamshield.gov.sg.
Make an appointment or seek a second opinion here.
The esophagus is the long, hollow tube that runs from your throat to your stomach and it carries food to the stomach to be digested. The wall of the esophagus comprises of several layers of tissue, including the mucous membrane, muscle, and connective tissue. The esophagus and stomach are part of the upper gastrointestinal (digestive) system.
Esophageal cancer usually begins in the cells lining the inside of the esophagus before spreading outwards through the other layers as it grows.
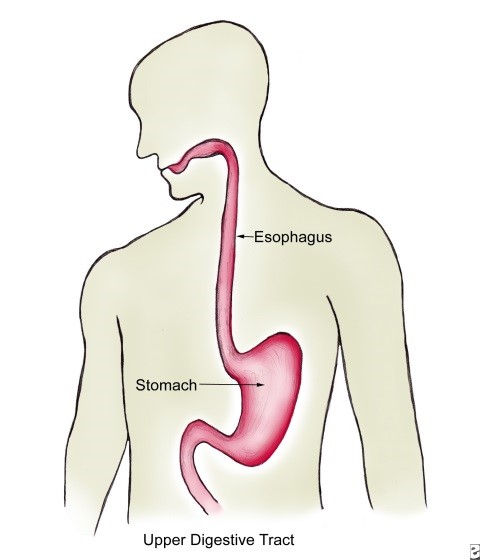
The two most common forms of esophageal cancer are:
*People who think they may be at risk should discuss this with their doctor.
*A doctor should be consulted if the above symptoms occur.
If you experience any of the symptoms mentioned, your doctor may refer you to a specialist after asking about your personal and family medical history and conducting a physical examination.
The following tests are used to diagnose esophageal cancer.
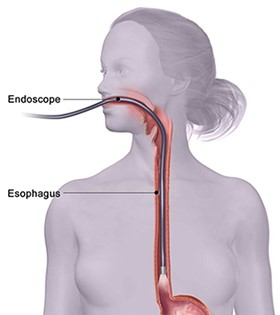
A hollow tube equipped with a lens (endoscope) will be passed down your throat and into your esophagus. Your doctor will then examine your esophagus for abnormalities or areas of irritation. Endoscope also provides the opportunity to remove a piece of tissue or sample (biopsy) from your esophagus. The tissue samples will then be sent to a laboratory to test for cancerous cells. Endoscopy ultrasound (EUS) is procedure that combines endoscopy and ultrasound to obtain images from your esophagus for investigations and staging.
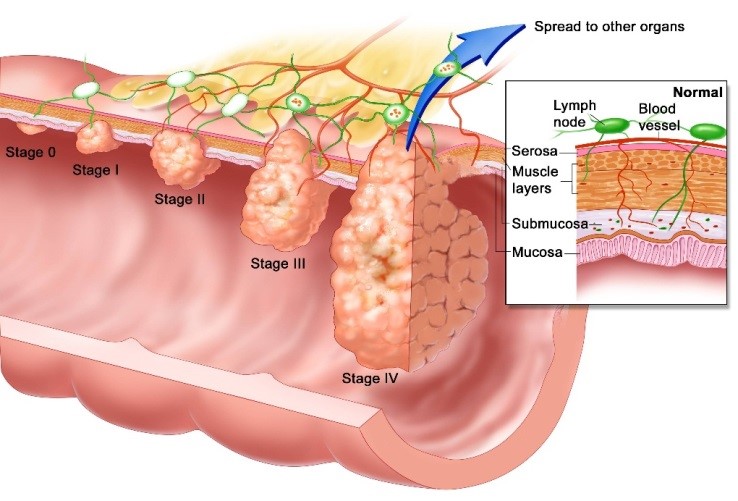
In the event that you are diagnosed with esophageal cancer, your doctor will then work to determine the stage of the cancer. Staging the cancer helps determine the most suitable treatment options. Find out more about the different stages of esophageal cancer below.
Stage I - The cancer occurs in the superficial layers of cells lining the esophagus.
Stage II - The cancer has progressed to deeper layers of the esophagus lining and may have spread to nearby lymph nodes.
Stage III - The cancer has spread to the deepest layers of the esophagus wall and to nearby tissues or lymph nodes.
Stage IV- The cancer has spread to other parts of the body.
There are different treatments available for esophageal cancer depending on the stage, type and the position of the cancer. Factors other than the stage of the cancer that might have an impact on your treatment decision include your age, your overall health, and your own preferences. The three main types of treatment include surgery, radiation and chemotherapy.
Surgery
Surgery is the most common treatment option for esophageal cancer.
Chemotherapy
Chemotherapy is the use of drugs to help kill cancer cells and shrink the size of the tumour. It can be given alone or combined with radiotherapy before or after surgery. It is also the treatment of choice if the patient is not suitable for surgery. The drugs are given into a vein or by mouth. Once the drugs enter the bloodstream, they spread throughout the body. In esophageal cancer, multiple chemotherapy sessions are usually required.
Radiation Therapy
Radiation therapy uses high-powered energy beams to kill cancer cells. Radiation can come from a machine outside your body that aims the beams at your cancer (external beam radiation) or it can be placed inside your body near the cancer (brachytherapy).
Radiation therapy is commonly combined with chemotherapy in the treatment of esophageal cancer. It can be used before or after surgery. Radiation therapy is also used to relieve complications of advanced esophageal cancer, for example, in cases where the tumour grows large enough to obstruct food from passing through your stomach.

Esophageal Cancer Care Approach

Esophageal Cancer Care Team

Esophageal Cancer Online Resource Library

Patient Support Groups

Esophageal Cancer Clinical Trials