AccordionContent1
 Cancer is a family affair. Our loved ones go through intense physical and emotional ups and downs throughout the diagnosis, treatment, and recovery phases of cancer. However, cancer caregivers experience a separate set of worries and difficult emotions that are often not addressed or dealt with properly. This section focuses on caregivers’ reactions to the diagnosis of a loved one, providing you with tips on various ways to address the fear of uncertainty.
Cancer is a family affair. Our loved ones go through intense physical and emotional ups and downs throughout the diagnosis, treatment, and recovery phases of cancer. However, cancer caregivers experience a separate set of worries and difficult emotions that are often not addressed or dealt with properly. This section focuses on caregivers’ reactions to the diagnosis of a loved one, providing you with tips on various ways to address the fear of uncertainty.
Various reactions to a diagnosis of cancer are normal, and are affected by your relationship with your loved one. Whether you are a spouse, child, sibling, relative, or close friend of your loved one, you may experience varying reactions.
Normal caregiver reactions to their loved one's cancer diagnosis include:
-
Denial, shock, anxiety, worry, disbelief, anger
-
Existential questions
-
Practical concerns e.g. finances, family function, disability
-
Dependent on stage of diagnosis - tumour, metastases, prognosis, treatment trajectory
So, as a caregiver, what can you do to cope with feelings of worry or uncertainty about the future? Here are some tips:
Be patient
Give yourself time to come to terms with it as a caregiver and take things one step at a time.
Acceptance
Recognise and accept that there may be difficult times ahead, however, this does not mean losing hope and letting negative feelings consume you.
Review lifestyles and priorities
Be flexible, put non-urgent or unimportant things on hold.
Be proactive
Find out about the treatment pathway and options available for your loved one.
Remain in the present moment
Practice 'mindfulness' and don't let your mind wander too far into the future too often. Do what you can within your control and try to let go of those things that you cannot control.
Attend classes/programmes on caregiving
This will allow you to interact and bond with other caregivers to share and gain insight on each other's caregiving experience. At the NCIS, we currently offer a training programme for caregivers known as Caregivers in Cancer. For more information, click here.
Engage support networks
Be it via your family, friends, spiritual/religious support or professional/counselling network and maintain open communication with your loved ones.
Lead an active life
Exercise helps to rejuvenate the body and mind and helps you sleep better. It is recommended to aim for at least 2 and a half hours of moderate activity a week. To find out more on how you can keep active, click here.
Have a healthy diet
During your caregiving journey, you may be too busy caring for your loved one and neglect your own nutritional needs. Eating right will strengthen your immune system and keep you energised throughout the day. Not sure what meals to prepare? You can save time by preparing the same nutritious meals for yourself and your loved one. To get some cooking inspiration, you can download our dietitian endorsed fuss-free healthy recipes suitable for cancer patients here.
Get ample rest
Sleep is an important part of your daily routine not to be neglected. If you are unable to get proper sleep at night, try to take naps during the day. Also, aim to get at least one full night's rest each week.
Make time for yourself
While caring for your loved one is important, caring for yourself is equally important. Allocate some time to do activities that you enjoy such as reading, listening to music, watching movies or playing sports. Try not to neglect your own personal life as well and engage in these activities with your friends.
Go for regular medical checkups
Sometimes, in the process of caregiving, you may overwork or wear yourself out. To ensure a clean bill of health, don't forget to go for regular health and dental checkups. Also, lookout for signs for anxiety or depression that occur. If you are affected, click here for tips on how to cope with it or alternatively, you can speak to a doctor about your condition.
Spirituality
Find meaning in the situation.
AccordionContent2
Caregivers often struggle with unhelpful and negative thoughts during their caregiving process that affects them in various ways. Some examples include:
- "I'm not doing a good job."
- "I should try harder."
- "The treatment is not going well. Something must be wrong."
- "What will happen to me or my family if my loved one passes away?"
- "It is my fault that he/she is feeling this way."
- "Bad things always happen to me."
As a caregiver, ask yourself what are some of the unhelpful thoughts that frequently occupy your mind. How do your thoughts control you, and how to they interact with other parts of yourself? Imagine this scenario with your eyes closed.
“You are walking down the street and you see someone you know on the other side. You smile and wave, but the person does not seem to notice you and keeps on walking.”
What are your initial (automatic) thoughts? What emotions are present? How might you behave afterwards?
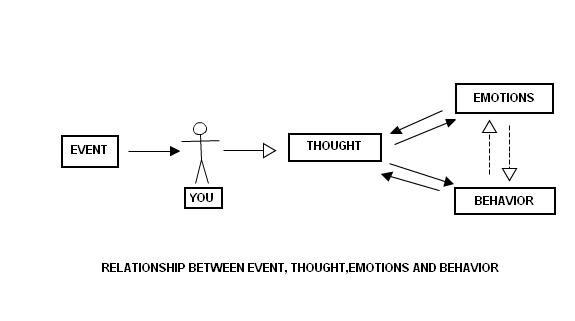
- It is not the event/situation itself, but our interpretation about it that determines our thoughts, mood and subsequent behaviour
- If we change our interpretation about the event, we can change the way we feel and react to the event
Sometimes, our thoughts can be inaccurate and unhelpful so you don't have to believe them. Here are some common unhelpful thinking habits we all make from time to time.

Now that you've identified your unhelpful thoughts, learn to replace them with alternative, more balanced thoughts. Here are some examples:
|
Critical - I am doing such a bad job and my loved one is angry with me. | I am doing my best. He/she must be having a hard time as well and does not mean it. |
|
Compare & Despair - Why do other patients seem to be getting better and not my loved one? | Everybody has their good and bad days, treatment is not the same for everybody. |
|
Shoulds & Musts - I should be available 24 hours a day and I must be able to help whenever he/she needs me. | Nobody can be available all the time; it is ok for me to take a rest. |
|
Black & White Thinking - If he/she is not well, there is no way we can have a normal family life. | He/she may not be in the best of health, but we can still do things together as a family. |
|
Catastrophising - Oh dear, he/she is having a cough, something must be wrong. I'd better send him/her to the hospital immediately. | It may not be anything serious. I'll not jump to conclusions and will investigate it calmly and properly. |
Eliminate Negative Thinking!
Through practicing these cognitive strategies, you can reduce the impact of negative and unhelpful thoughts on your behaviour and mood.
By looking at your thoughts rationally and calmly, you can then choose your actions in line with your values rather than letting unhelpful automatic thoughts control your life.
AccordionContent3
When our loved ones are ill, as caregivers, we have the natural tendency to want to make them feel better. We may go the extra mile to comfort them, bring them food that they like, or help them to carry out errands and tasks. Although we may have good intentions at heart, we may unknowingly overstretch ourselves by constantly putting others’ needs before ours.
Being a caregiver is an extremely stressful experience in itself, and we need to remember to take equally good care of ourselves in order to be in the best position to help our loved one. How do you know when you are under stress? Here are some symptoms you can spot for:
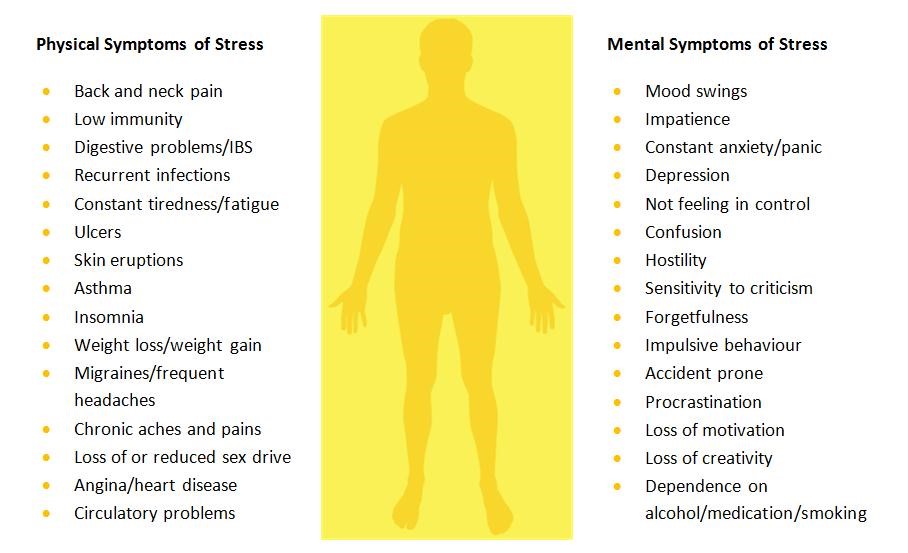
Self-Care & Relaxation
It is not selfish nor does it make you a poor caregiver if you take some time-off for yourself. The skill of "looking after ourselves" and paying attention to your needs is an important one. Here are some ideas to increase your self-care:
- Enjoying your favourite meal slowly
- Relaxing in a warm bath or shower
- Prayer and reflection
- Maintain a healthy balanced diet
- Take pride in your appearance e.g. going for a haircut etc
- Stop rushing around – you achieve more by doing things calmly
- Give yourself short breaks during the day – relax, stretch, go for a walk
- Plan a holiday or outing
- Visit a place of interest
- Do a crossword or a puzzle
- Visit close friends or relatives
- Listen to uplifting music or sing
Other Stress Management Tips
Emotional Acceptance
- Recognise your major sources of stress
- Be assertive - learn to say "no" to unnecessary tasks
- Adopt a systematic problem-solving approach - break your goals into smaller portions
- Recognise and accept your own feelings
- Reduce demands - don't expect too much of yourself and don't feel that you have to live up to others' expectations of you
Calm Breathing

Calm breathing (sometimes called deep diaphragmatic breathing) involves taking smooth, slow, and regular breaths. It is especially effective when you feel anxious, worried, or have physical symptoms of stress such as heart palpitations or sweaty palms.
- Take a comfortable sitting position and close your eyes if you are comfortable.
- Imagine that you have a balloon in your tummy. Every time you breathe in, the balloon inflates. Each time you breathe out, the balloon deflates.
- Take a slow breath in through the nose, breathing into your lower belly (for a count of 3)
- Exhale slowly through the nose (or mouth) for a count of 3.
- As you exhale, you may choose to say the word ‘relax’ to yourself in your mind.
- Repeat the cycle for approximately 10 times or until you feel more relaxed.
- Return to normal breathing for about a minute before you get up and carry on.
Progressive Muscle Relaxation (PMR)
One of the body's reactions to fear and anxiety is muscle tension. Muscle relaxation can be particularly helpful in cases where anxiety is especially associated with muscle tension.
One method of reducing muscle tension that people have found helpful is through a technique called Progressive Muscle Relaxation (PMR). Through PMR exercises, you tense up particular muscles then relax them, and practice this technique consistently.
Steps to Prepare
- Select your surroundings. Minimise distraction to your five senses such as by switching off the TV and radio, and using soft lighting.
- Make yourself comfortable. Use a chair that comfortably seats your body, including your head. Wear loose clothing and take off your shoes.
- Avoid practicing after heavy and big meals and do not practice after consuming any intoxicants, such as alcohol.
*Kindly note that if you have any injuries or a history of physical problems that may cause muscle pain, always consult your doctor before practicing these exercises.
Things to Note
- Once you have set aside the time and place for relaxation, slow down your breathing and give yourself permission to relax.
- When you are ready to begin, tense the muscle group described. Make sure you can feel the tension, but not so much that you feel a great deal of pain. Keep the muscle tensed for approximately five seconds.
- Relax the muscle and keep it relaxed for approximately ten seconds. It may be helpful to say something like "Relax" as you relax the muscle.
- When you have finished the relaxation procedure, remain seated for a few moments allowing yourself to become alert.
Step-by-step Guide
-
Right hand and forearm - Make a fist with your right hand.
-
Right upper arm - Bring your right forearm up to your shoulder to "make a muscle".
-
Left hand and forearm - Repeat as per right hand and forearm.
-
Left upper arm - Repeat as per right hand and forearm.
-
Forehead - Raise your eyebrows as high as they will go, as though you are surprised by something.
-
Eyes and cheeks - Squeeze your eyes tightly shut.
-
Mouth and jaw - Open your mouth as wide as you can, as though you are yawning.
-
Neck - Be careful as you tense these muscles. Put your face forward then pull your head back slowly, looking up towards the ceiling.
-
Shoulders - Tense the muscles in your shoulders as you bring your shoulders up towards your ears.
- Shoulder blades/Back - Push your shoulder blades back, trying to almost touch them together, so that your chest is pushed forward.
-
Chest and stomach - Breathe in deeply, filling up your lungs and chest with air.
-
Hips and buttocks - Squeeze your buttock muscles.
-
Right upper leg - Tighten your right thigh.
-
Right lower leg - Do this slowly and carefully to avoid cramps. Pull your toes towards you to stretch the calf muscle. Do this slowly and carefully to avoid cramps.
-
Right foot - Curl your toes downwards.
-
Left upper leg - Repeat as per right upper leg.
-
Left lower leg - Repeat as per right lower leg.
-
Left foot - Repeat as per right foot.
Practice means progress. Only through practice can you become more aware of your muscles, how they respond to tension and how you can relax them.
AccordionContent4
Cancer caregivers tend to experience strong emotions during the cancer journey with their loved ones. This can range from sadness, worry, fear, guilt, anger, and frustration. As a caregiver, what can you do to handle this emotional reactivity when it arises?
These are some tips to help you cope better.
Distraction helps you feel better by diverting your attention away from the distressing thoughts & feelings. It works even better if you choose something that will really grab your attention and keep you absorbed in that activity. Different things work for different people. Here are some ideas:
Self-soothing works when you are emotionally charged to provide yourself with comfort, nurturing and to be kind to yourself. One way to think of this is to soothe each of your five senses via the following methods below.

AccordionContent5
Taking care of a loved one with cancer may be overwhelming and sometimes, it may cause physical and mental exhaustion, sometimes even leading up to anxiety and depression that are not to be taken lightly. Read up on the signs of anxiety and depression so as to recognise the warning signs early and get tips on how to deal with them.
If you are going through anxiety and/or depression and need to speak to someone about it, do contact our CancerLine hotline, a free and anonymous counselling hotline operated by trained oncology nurses at +65 9722 0569 who will be able to assist you with your situation.
Anxiety
Anxiety is a common emotion that anyone can experience in their everyday lives. It occurs in response to perceived threats and can present as physical, emotional and behavioural reactions.
However, anxiety starts becoming a problem when it:
- Affects daily life
- Increases in intensity and/or duration
- Causes unexplained physical symptoms
- Leads to avoidance of situations and places
The term "Anxiety Disorders" includes Generalised Anxiety Disorder, Obsessive Compulsive Disorder, Phobias, Acute and Post-traumatic Stress Disorder. Although anxiety is a common feature and the different types of anxiety disorders have different symptoms, generally, all respond well to treatment.
How do I relieve anxiety?
These are some tips that may help:
- Be positive in your thoughts
- Feel good about your efforts and accomplishments
- Accept yourself and don't be self-critical
- Be flexible and be open to the grey area of things
- Develop realistic goals and work towards them
- Nurture your spirituality
- Distract yourself from stressors and take time to relax
- Deep breathing, relaxation, mediation, or visualisation
- Finding humour in things
- Spending time with people you enjoy
- Keep a journal for venting, and close the entry with something positive
- Take time regularly to do activities that you enjoy
- Utilise your support system
- Practice being assertive
- Take short breaks through the day to remove yourself from stressors and demands
- Get adequate rest and sleep
- Practice good nutrition
- Get a massage to relieve muscle tension and relax
- Choose to be in environments that feel good to you
- Work on your financial security
- Practice good time management
- Practice good communication
- Exercise regularly
- Do things that demonstrate respect, care, and nurturing of self
- Take good care of yourself
- Develop a self-care plan that will form your new and healthy lifestyle
Anxiety Management Tips
Practise Positive Self-Statements
Preparation
- It's not going to be as bad as I think
- It won't last long and I can cope with it
- I'm getting better and need to rebuild my confidence
- If I do get bad feelings, I know they won't last long and I can cope with them
- It's better to go than not to go, worrying doesn't help
- I might enjoy it if I go
Coping
- Concentrate on what is going on
- This is just anxiety; it is an unpleasant feeling but it won't make me ill
- These feelings are unpleasant but not harmful or dangerous
- I can tolerate anxiety, I have managed it many times before
- One step at a time
- Concentrate on what I have to do
- Remember to relax and think positive
- I know I'm going to be OK
- The feelings always fade
Praise / Review
- If I keep this up, I'm going to get really good at this
- I handled that so it should be easier next time
- I did that well
- I can be pleased with the progress I'm making
- I coped with that
- I have achieved my goal, I'm getting better
AccordionContent6
Depression is a word used in everyday language to describe a number of feelings, including sadness, frustration, disappointment, and sometimes lethargy. However, the clinical definition differs from these everyday "down" periods in three main ways:
- It is more intense
- It lasts longer
- It significantly interferes with effective day-to-day functioning
Depression can affect anybody at any stage of their life.
What are the symptoms?
- Low mood - Individuals will usually feel low for more than two weeks, depending on the severity of depression. Depression can be classified into mild depression and severe depression. In addition to stress, another mood common to depression is anxiety.
- Negative thoughts - Normally, individuals who are depressed have a negative outlook of life, a sense of guilt and low self-esteem and confidence.
- Physical symptoms
- Possible change in sleep patterns - Difficulty falling asleep or have interrupted sleep. Others sleep more and have difficulty staying awake or have early awakenings
- Possible changes in appetite and weight - Some may experience appetite and weight loss while others eat more than usual
- Possible decline in sexual interest
- Fall in energy levels - Constantly feeling lethargic and tired
- Disinterest - Lack of motivation to carry out everyday activities
- Daily interaction with people
- Unhappy and dissatisfied with family and other close ones
- Shy and anxious in a group settings
- Lonely and isolated yet unwilling or unable to reach out to others despite having opportunities to do so
What causes depression?
Depression is often caused by a combination of biological and psychological factors interacting with one another.
Biological Factors
- Genetic factors - Depression often runs in families, which suggest that individuals may inherit genes that make them vulnerable to developing depression; however, one may inherit an increased vulnerability to the illness, but not necessarily the illness itself. Although many people may inherit this vulnerability, a great many of them may never suffer a depressive illness.
- Hormones - Research has shown that there are some hormonal changes that may account for some symptoms of depression. Medication can effectively treat these conditions.
- Brain chemicals (neurotransmitters) - During depression, there is reduced activity of brain chemicals, and this disturbs certain areas of the brain that regulate functions such as sleep, appetite, sexual drive and mood. Many anti-depressant drugs increase the amount of brain chemicals.
Psychological Factors
- Thinking patterns associated with depression include:
- Overstressing the negative
- Taking responsibility for bad events but not for good events
- Having inflexible rules about how one should behave
- Thinking that you know what others are thinking and that they are thinking badly of you
- Loss of a loved one through bereavement or separation, loss of a job or friendship, loss of promotion or support etc
- Sense of failure
- Stress
Pharmacological (e.g. antidepressants) and psychological therapies are available and effective in treating depression.
Depression management tips
#1 Reversing the cycle of depression
- Medication - Anti-depressants improve the mood and sleep and can help change your energy level
- Set realistic and achievable goals - This can help you tackle your tasks and responsibilities with success
- Increasing your activity level - Take parts in activities you enjoy and feel happy doing
Here are some possible fun things you can do:
- Soaking in the bathtub
- Collecting things (coins, shells, etc)
- Going for a day trip
- Going to see a comedy
- Going to the beach
- Having a barbeque with family and/or friends
- Going for a walk or hike
- Listening to uplifting music
- Gardening
Try some of them out and evaluate how you feel before and after the activity. Chances are, you will find that you feel a little better. The important thing is to persist.
#2 Understanding yourself
What really makes us feel and respond the way we do is not the situation or the words and actions of another person, but how we perceive the situation or that person's actions. It is our thoughts and beliefs about an event that significantly influence our feelings and actions. We may not be aware of our thoughts and beliefs as they are often automatic and happen quickly.
If you are feeling anxious, depressed or upset, it is very likely that you have been thinking negative thoughts. These are called unhelpful thoughts as they lead to unpleasant feelings or actions. All of us think about things that make us feel sad or anxious, and that is part and parcel of life. However, if you often feel distressed or upset, you may ned to examine your thoughts in order to improve how you feel.
What are unhelpful thoughts?
Unhelpful thoughts are thought patterns that have become a habit and contribute to a person's negative feelings. Thoughts that are considered unhelpful are:
- Those that tend to focus on negativity
- Those that overestimate the chances of a negative event occurring
- Those that place unrealistic demands on yourself or others
Things you can do to make yourself feel better
- Identify how or what you are feeling to see how and why you are feeling distressed. Remember, unhelpful thoughts will lead to upsetting emotions.
- Challenge your thinking by exploring other possible explanations and looking at situations from different viewpoints.
- Replace your original unhelpful thoughts with positive and helpful beliefs.
AccordionContent7
AccordionContent8
AccordionContent9
AccordionContent10
AccordionContent11
AccordionContent12
