NUHS Institutions will NEVER ask you to transfer money or disclose bank details over a call.
If in doubt, call the 24/7 ScamShield helpline at 1799, or visit the ScamShield website at www.scamshield.gov.sg.
Make an appointment or seek a second opinion here.
Cervical cancer is cancer of the entrance to the uterus or womb. It starts when abnormal cells grow out of control in the transformation zone (the area where squamous cells and glandular cells meet).
The cells do not suddenly transform into cancer; the normal cells in the cervix slowly change, which then turn it into cancer instead.
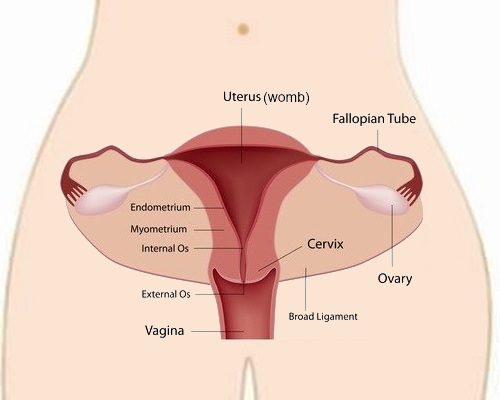
Long before there is cancerous growth on the cervix, the cells of the cervix undergo changes that will eventually lead to cancer. These changes in the cells of the cervix are known as cervical dysplastic changes or cervical pre-cancer. Slowly and over time the abnormal and dysplastic cells increase in number and take over more and more normal tissue. Eventually when the dysplastic cells breach an important tissue layer, the basement membrane, the dysplastic growth has formally become a cancer.
During the pre-cancerous phase of dysplastic change, there are no noticeable symptoms, and the only reliable way to detect these pre-cancerous changes is to have a series of pap smear tests. This is the main reason to recommend having regular pap smear tests. The other reason regular pap smear tests work is that the pre-cancerous phase of change in the cervix extends over a significant period of time. In some studies, it has been estimated that it could take up to 10 years from the time the first pre-cancerous cell appears to the time that there is cancer on the cervix.
The HPV vaccination works because the Human Papillomavirus is a key element in the development of cervical cancer. HPV is what is known as a DNA virus and although there are over 200 different subtypes, only a small handful are known as “high risk” HPV. They are known as “high risk” because if a woman is infected for a long time with a “high risk” HPV subtype it significantly increases the likelihood of her developing cervical cancer. There is a growing body of evidence that suggests that women who have never been exposed to HPV and who are vaccinated against it, have a much lower likelihood of ever developing cervical pre-cancer or cancer. HPV vaccines have been around for a sufficiently long time and with almost 200 million doses delivered worldwide, the World Health Organization has declared that the vaccine is safe and that all eligible women should consider vaccination. The HPV vaccination is also part of national vaccination programs for school children in countries such as Australia and Great Britain.
It is important at this point to emphasise that HPV infection is very common, almost like catching the common cold in humans, and that cervical cancer develops only in a very small percentage of the total number of HPV infections. The vast majority of women who are infected with HPV clear it effectively. The problem is that there is no effective way to know which women will effectively clear high-risk HPV and which won’t and among those that don’t clear the viral infection, which will go on to develop cervical cancer. That is why doctors recommend vaccination for EVERYBODY that is eligible.
With minimal effort, you can prevent cervical cancer effectively by getting your HPV vaccine and getting regular pap smear tests.
* People who think they may be at risk should discuss this with their doctor.
Cervical cancer may be associated with the following symptoms:
* A doctor should be consulted if the symptoms above occur.
There are two ways to prevent cervical cancer:
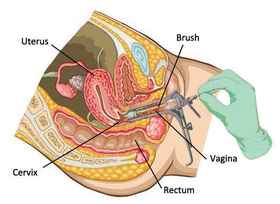
A pap smear test is a simple procedure where cells are collected from the surface of the cervix and then sent to a laboratory to detect any abnormality. All sexually active women between 25 and 69 years old are advised to have a pap smear test regularly (every 3 years on average).
The first step in finding out if you have cervical cancer, as doctors suggest, is through a pap test. During the test, the doctor gently scrapes the outside of the vagina and cervix to take samples of cells. The cells will then be taken to the laboratory for testing.
Other than a pap test, here are some other ways cervical cancer is diagnosed.
Colposcopy
If you have certain symptoms suggesting cancer your doctor may recommend a colposcopy. During the procedure, a speculum will be placed inside the vagina and use a colposcope to examine the cervix. The doctor will then apply a weak solution of acetic acid to the cervix to see any abnormal areas easily.
Cone Biopsy
During a biopsy, some tissue in the cervix will be removed for examination under a microscope. Other tests can only suggest cancer, but only a biopsy can give a clear-cut answer.
Depending on the stage of the cervical cancer, there are various treatment options available. Here are the main types of treatment.
Surgery
During a surgery, a surgical oncologist will remove the tumour and surrounding tissue. There are three main types of surgery for cervical cancer: (1) Radical trachelectomy, (2) Hysterectomy, and (3) Pelvic exenteration.
Radiation Therapy
Radiation therapy uses a high-dose of X-ray in the vagina to destroy the cancer cells. This type of therapy may be given alone, before surgery, or instead of surgery to shrink the tumour. Radiation therapy is particularly used for certain stages of cervical cancer.
Chemotherapy
Chemotherapy uses medicines to kill cancer cells. It may be used to treat advanced cervical cancer. Chemotherapy may be combined with radiotherapy to cure cervical cancer, or it can be used as the only treatment for advanced cervical cancer.

Cervial Cancer Care Approach

Cervical Cancer Care Team

Cervical Cancer Online Resource Library

Patient Support Groups

Condition Cancer Clinical Trials

Warna 94.2FM Radio Show with Dr Ida

Cervical Cancer Resesarch